
| Tracking the next pandemic: Avian Flu Talk |
MERS-CoV WHO updates |
Post Reply 
|
| Author | |
Kyle 
Adviser Group 
Joined: May 29 2013 Location: Colorado, USA Status: Offline Points: 5800 |
 Post Options Post Options
 Thanks(0) Thanks(0)
 Quote Quote  Reply Reply
 Topic: MERS-CoV WHO updates Topic: MERS-CoV WHO updatesPosted: April 21 2014 at 8:09am |
|
20/04/2014 20 April 2014 - On 18 April 2014, the Ministry of Health of Greece reported one laboratory-confirmed case of infection with Middle East respiratory syndrome coronavirus (MERS-CoV). The following details were provided to WHO by the Ministry of Health, Greece, on 18 April 2014: The patient is a 69-year old male Greek citizen residing in Jeddah, Saudi Arabia, who travelled back to Greece on 17 April. While in Jeddah, the patient consulted a hospital on 8 and 10 April for a febrile illness with diarrhoea, and was given a probable diagnosis of typhoid fever. Of note, he regularly visited his wife who was hospitalised from 31 March to 5 April in the same hospital for a confirmed typhoid fever. The patient sought medical care upon arrival in Greece on 17 April. The evaluation revealed a bilateral pneumonia and the diagnosis of MERS-CoV infection was made at the National Reference Laboratory for Influenza. The patient is in stable condition and is receiving appropriate treatment. This is the first case of MERS-CoV infection in the country. Individuals who had close contacts with the case in the plane, the hospital in Greece and in the community have been identified and are being followed up. So far, none of the contacts became ill. Hellenic health authorities issued a press release to inform the population and informed all Greek hospitals on measures that need be taken to identify suspect patients and implement appropriate preventive measures. Globally, from September 2012 to date, WHO has been informed of a total of 250 laboratory-confirmed cases of infection with MERS-CoV, including 93 deaths. WHO advice Based on the current situation and available information, WHO encourages all Member States to continue their surveillance for severe acute respiratory infections (SARI) and to carefully review any unusual patterns. Infection prevention and control measures are critical to prevent the possible spread of MERS-CoV in health care facilities. Health-care facilities that provide for patients suspected or confirmed to be infected with MERS-CoV infection should take appropriate measures to decrease the risk of transmission of the virus from an infected patient to other patients, health-care workers and visitors. Health care workers should be educated, trained and refreshed with skills on infection prevention and control. It is not always possible to identify patients with MERS-CoV early because some have mild or unusual symptoms. For this reason, it is important that health-care workers apply standard precautions consistently with all patients – regardless of their diagnosis – in all work practices all the time. Droplet precautions should be added to the standard precautions when providing care to all patients with symptoms of acute respiratory infection. Contact precautions and eye protection should be added when caring for probable or confirmed cases of MERS-CoV infection. Airborne precautions should be applied when performing aerosol generating procedures. Patients should be managed as potentially infected when the clinical and epidemiological clues strongly suggest MERS-CoV, even if an initial test on a nasopharyngeal swab is negative. Repeat testing should be done when the initial testing is negative, preferably on specimens from the lower respiratory tract. Health-care providers are advised to maintain vigilance. Recent travellers returning from the Middle East who develop SARI should be tested for MERS-CoV as advised in the current surveillance recommendations. All Member States are reminded to promptly assess and notify WHO of any new case of infection with MERS-CoV, along with information about potential exposures that may have resulted in infection and a description of the clinical course. Investigation into the source of exposure should promptly be initiated to identify the mode of exposure, so that further transmission of the virus can be prevented. People at high risk of severe disease due to MERS-CoV should avoid close contact with animals when visiting farms or barn areas where the virus is known to be potentially circulating. For the general public, when visiting a farm or a barn, general hygiene measures, such as regular hand washing before and after touching animals, avoiding contact with sick animals, and following food hygiene practices, should be adhered to. WHO does not advise special screening at points of entry with regard to this event nor does it currently recommend the application of any travel or trade restrictions. WHO |
|
 |
|
Satori 
Valued Member 
Joined: June 03 2013 Status: Offline Points: 28655 |
 Post Options Post Options
 Thanks(0) Thanks(0)
 Quote Quote  Reply Reply
 Posted: April 21 2014 at 2:59pm Posted: April 21 2014 at 2:59pm |
|
Saudi Arabia Removes Health Minister as Deadly Virus Spreads |
|
 |
|
Kyle 
Adviser Group 
Joined: May 29 2013 Location: Colorado, USA Status: Offline Points: 5800 |
 Post Options Post Options
 Thanks(0) Thanks(0)
 Quote Quote  Reply Reply
 Posted: April 24 2014 at 8:35am Posted: April 24 2014 at 8:35am |
|
Middle East respiratory syndrome coronavirus (MERS-CoV) – update
Disease Outbreak News 24 APRIL 2014 - On 22 April 2014, the Ministry of Health of Jordan reported an additional laboratory-confirmed case of infection with Middle East respiratory syndrome coronavirus (MERS-CoV). The patient is a 25 year-old man from Al Grayat City, Saudi Arabia. He became ill on 9 April, was admitted to a hospital in Saudi Arabia on 10 April and discharged from the hospital on 15 April, against medical advice. As his condition did not improve, he sought medical care at another hospital in Zarka City, Jordan on 19 April, where he was tested positive for MERS-CoV. The patient has underlying medical conditions and has a history of travel to Abha Mecca and Jeddah, Saudi Arabia from 3 to 8 April. He has history of contact with camels and is also reported to have consumed camel milk. Globally, from September 2012 to date, WHO has been informed of a total of 254 laboratory-confirmed cases of infection with MERS-CoV, including 93 deaths. WHO advice Based on the current situation and available information, WHO encourages all Member States to continue their surveillance for severe acute respiratory infections (SARI) and to carefully review any unusual patterns. Infection prevention and control measures are critical to prevent the possible spread of MERS-CoV in health care facilities. Health-care facilities that provide for patients suspected or confirmed to be infected with MERS-CoV infection should take appropriate measures to decrease the risk of transmission of the virus from an infected patient to other patients, health-care workers and visitors. Health care workers should be educated, trained and refreshed with skills on infection prevention and control. It is not always possible to identify patients with MERS-CoV early because some have mild or unusual symptoms. For this reason, it is important that health-care workers apply standard precautions consistently with all patients – regardless of their diagnosis – in all work practices all the time. Droplet precautions should be added to the standard precautions when providing care to all patients with symptoms of acute respiratory infection. Contact precautions and eye protection should be added when caring for probable or confirmed cases of MERS-CoV infection. Airborne precautions should be applied when performing aerosol generating procedures. Patients should be managed as potentially infected when the clinical and epidemiological clues strongly suggest MERS-CoV, even if an initial test on a nasopharyngeal swab is negative. Repeat testing should be done when the initial testing is negative, preferably on specimens from the lower respiratory tract. Health-care providers are advised to maintain vigilance. Recent travellers returning from the Middle East who develop SARI should be tested for MERS-CoV as advised in the current surveillance recommendations. All Member States are reminded to promptly assess and notify WHO of any new case of infection with MERS-CoV, along with information about potential exposures that may have resulted in infection and a description of the clinical course. Investigation into the source of exposure should promptly be initiated to identify the mode of exposure, so that further transmission of the virus can be prevented. People at high risk of severe disease due to MERS-CoV should avoid close contact with animals when visiting farms or barn areas where the virus is known to be potentially circulating. For the general public, when visiting a farm or a barn, general hygiene measures, such as regular hand washing before and after touching animals, avoiding contact with sick animals, and following food hygiene practices, should be adhered to. WHO does not advise special screening at points of entry with regard to this event nor does it currently recommend the application of any travel or trade restrictions. WHO |
|
 |
|
Kyle 
Adviser Group 
Joined: May 29 2013 Location: Colorado, USA Status: Offline Points: 5800 |
 Post Options Post Options
 Thanks(0) Thanks(0)
 Quote Quote  Reply Reply
 Posted: April 27 2014 at 12:11pm Posted: April 27 2014 at 12:11pm |
|
Middle East respiratory syndrome coronavirus (MERS-CoV) – update
26/04/2014 On 26 April 2014, the Ministry of Health of the United Arab Emirates (UAE) reported seven additional laboratory-confirmed cases of infection with Middle East Respiratory Syndrome coronavirus (MERS-CoV). The following details were provided to WHO on 24 April 2014:
To date, all the abovementioned cases are in isolation in a hospital and are well. Screening of other contacts within the health care setting and families are ongoing. Globally, from September 2012 to date, WHO has been informed of a total of 261 laboratory-confirmed cases of infection with MERS-CoV, including 93 deaths. Based on the current situation and available information, WHO encourages all Member States to continue their surveillance for severe acute respiratory infections (SARI) and to carefully review any unusual patterns. Infection prevention and control measures are critical to prevent the possible spread of MERS-CoV in health care facilities. Health-care facilities that provide for patients suspected or confirmed to be infected with MERS-CoV infection should take appropriate measures to decrease the risk of transmission of the virus from an infected patient to other patients, health-care workers and visitors. Health care workers should be educated, trained and refreshed with skills on infection prevention and control. It is not always possible to identify patients with MERS-CoV early because some have mild or unusual symptoms. For this reason, it is important that health-care workers apply standard precautions consistently with all patients – regardless of their diagnosis – in all work practices all the time. Droplet precautions should be added to the standard precautions when providing care to all patients with symptoms of acute respiratory infection. Contact precautions and eye protection should be added when caring for probable or confirmed cases of MERS-CoV infection. Airborne precautions should be applied when performing aerosol generating procedures. Patients should be managed as potentially infected when the clinical and epidemiological clues strongly suggest MERS-CoV, even if an initial test on a nasopharyngeal swab is negative. Repeat testing should be done when the initial testing is negative, preferably on specimens from the lower respiratory tract. Health-care providers are advised to maintain vigilance. Recent travellers returning from the Middle East who develop SARI should be tested for MERS-CoV as advised in the current surveillance recommendations. All Member States are reminded to promptly assess and notify WHO of any new case of infection with MERS-CoV, along with information about potential exposures that may have resulted in infection and a description of the clinical course. Investigation into the source of exposure should promptly be initiated to identify the mode of exposure, so that further transmission of the virus can be prevented. People at high risk of severe disease due to MERS-CoV should avoid close contact with animals when visiting farms or barn areas where the virus is known to be potentially circulating. For the general public, when visiting a farm or a barn, general hygiene measures, such as regular hand washing before and after touching animals, avoiding contact with sick animals, and following food hygiene practices, should be adhered to. WHO does not advise special screening at points of entry with regard to this event nor does it currently recommend the application of any travel or trade restrictions. |
|
 |
|
Kyle 
Adviser Group 
Joined: May 29 2013 Location: Colorado, USA Status: Offline Points: 5800 |
 Post Options Post Options
 Thanks(0) Thanks(0)
 Quote Quote  Reply Reply
 Posted: April 29 2014 at 8:27am Posted: April 29 2014 at 8:27am |
WHO scientists head to Saudi Arabia to help with MERS outbreak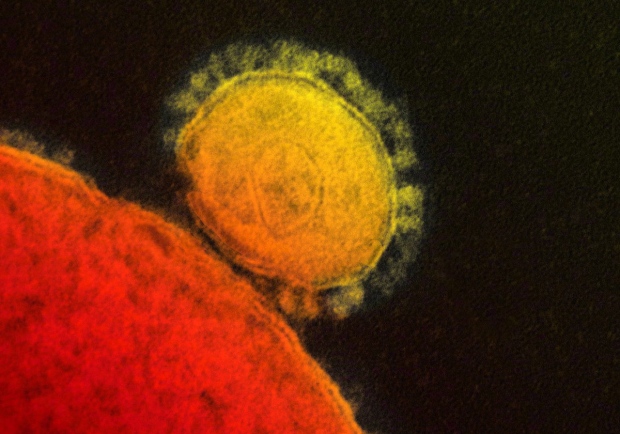 A colourized transmission of the MERS coronavirus that emerged in 2012 is shown. (THE CANADIAN PRESS/HO, National Institute for Allergy and Infectious Diseases) TORONTO -- Scientists from the World Health Organization are travelling to Saudi Arabia to help investigate this month's large increase in cases of MERS -- Middle East respiratory syndrome. A spokesperson for the Geneva-based agency says the mission is a response to a request for assistance from the Saudi government. The number of MERS infections has soared recently, with more cases being diagnosed this month alone than in the past two years combined. more: http://www.ctvnews.ca/health/who-scientists-head-to-saudi-arabia-to-help-with-mers-outbreak-1.1797159#ixzz30HzmndkF |
|
 |
|
coyote 
Admin Group 
Joined: April 25 2007 Location: United States Status: Offline Points: 8395 |
 Post Options Post Options
 Thanks(0) Thanks(0)
 Quote Quote  Reply Reply
 Posted: April 30 2014 at 9:00am Posted: April 30 2014 at 9:00am |
|
WHO: Upsurge in MERS Corona Virus Due to Warmer Weather
GENEVA — The World Health Organization (WHO) says it believes the recent spike in cases of Middle East Respiratory Syndrome, or MERS Corona virus is probably due to a seasonal increase of the disease rather than to any changes in the behavior of the virus. WHO says similar upsurges have occurred around the same time in the past two years. WHO spokesman Gregory Hartl says the increase in cases is most likely due to the warmer weather in the Arabian Peninsula and to outbreaks of the disease in two or three hospitals in Saudi Arabia and the United Arab Emirates. [link to www.voanews.com] |
|
|
Long time lurker since day one to Member.
|
|
 |
|
Kyle 
Adviser Group 
Joined: May 29 2013 Location: Colorado, USA Status: Offline Points: 5800 |
 Post Options Post Options
 Thanks(0) Thanks(0)
 Quote Quote  Reply Reply
 Posted: May 05 2014 at 12:00pm Posted: May 05 2014 at 12:00pm |
Middle East respiratory syndrome coronavirus (MERS-CoV) – updateDisease Outbreak News 5 MAY 2014 - On 2 May 2014, the US IHR National Focal Point reported the first laboratory confirmed Middle East respiratory syndrome coronavirus (MERS-CoV) infection in a male US citizen in his 60s, who lives and works in Riyadh, Saudi Arabia. He traveled to the US from Riyadh to Chicago on 24 April 2014 via London Heathrow with travel from Chicago to Indiana by bus. He reportedly worked in Riyadh. US health officials do not know at this time whether he directly cared for MERS-CoV confirmed cases and what infection control precautions were used. The CDC Team is working with the Indiana State Health Department to collect more data on the patient, including this information. He began feeling unwell on or around 14 April 2014 with a low-grade fever without any respiratory symptoms. On 27 April 2014, he developed shortness of breath, cough, increasing fever, and mild runny nose. On 28 April 2014, he was seen in an emergency room. A chest x-ray showed infiltrates in the right lung base and he was admitted to hospital and placed in a private room. Negative pressure room and airborne precautions were reportedly implemented on 29 April 2014; full isolation (standard, contact, and airborne) precautions were implemented on 30 April 2014. A chest computed tomography on 29 April 2014 showed bilateral lung infiltrates. Currently the patient is stable with shortness of breath; he is not intubated. CDC’s Division of Global Migration and Quarantine (DGMQ) has been and continues to work with local, state, and international partners, as well as airlines and the bus company to obtain the passenger manifests from the two flights and information from the bus company to help identify, locate, and interview contacts. This is the first report of an imported case of MERS-CoV in the United States and in the Americas Region. WHO adviceBased on the current situation and available information, WHO encourages all Member States to continue their surveillance for severe acute respiratory infections (SARI) and to carefully review any unusual patterns. Infection prevention and control measures are critical to prevent the possible spread of MERS-CoV in health care facilities. Health-care facilities that provide for patients suspected or confirmed to be infected with MERS-CoV infection should take appropriate measures to decrease the risk of transmission of the virus from an infected patient to other patients, health-care workers and visitors. Health care workers should be educated, trained and refreshed with skills on infection prevention and control. It is not always possible to identify patients with MERS-CoV early because some have mild or unusual symptoms. For this reason, it is important that health-care workers apply standard precautions consistently with all patients – regardless of their diagnosis – in all work practices all the time. Droplet precautions should be added to the standard precautions when providing care to all patients with symptoms of acute respiratory infection. Contact precautions and eye protection should be added when caring for probable or confirmed cases of MERS-CoV infection. Airborne precautions should be applied when performing aerosol generating procedures. Patients should be managed as potentially infected when the clinical and epidemiological clues strongly suggest MERS-CoV, even if an initial test on a nasopharyngeal swab is negative. Repeat testing should be done when the initial testing is negative, preferably on specimens from the lower respiratory tract. Health-care providers are advised to maintain vigilance. Recent travellers returning from the Middle East who develop SARI should be tested for MERS-CoV as advised in the current surveillance recommendations. All Member States are reminded to promptly assess and notify WHO of any new case of infection with MERS-CoV, along with information about potential exposures that may have resulted in infection and a description of the clinical course. Investigation into the source of exposure should promptly be initiated to identify the mode of exposure, so that further transmission of the virus can be prevented. People at high risk of severe disease due to MERS-CoV should avoid close contact with animals when visiting farms or barn areas where the virus is known to be potentially circulating. For the general public, when visiting a farm or a barn, general hygiene measures, such as regular hand washing before and after touching animals, avoiding contact with sick animals, and following food hygiene practices, should be adhered to. WHO does not advise special screening at points of entry with regard to this event nor does it currently recommend the application of any travel or trade restrictions. http://www.who.int/csr/don/2014_05_05_mers/en/ |
|
 |
|
Elver 
Valued Member 
Joined: June 14 2008 Status: Offline Points: 7778 |
 Post Options Post Options
 Thanks(0) Thanks(0)
 Quote Quote  Reply Reply
 Posted: May 05 2014 at 9:11pm Posted: May 05 2014 at 9:11pm |
|
It's only a matter of time. Perhaps these healthcare workers from Africa and the middle east should self-quarantine prior to returning home.
We have H5N1, H3N2, H7N9, H1N1, MERS-CoV, Ebola, MRSA, C Diff, and the various forms of TB. How can all of these strike at the same time? |
|
 |
|
CRS, DrPH 
Expert Level Adviser 
Joined: January 20 2014 Location: Arizona Status: Offline Points: 26660 |
 Post Options Post Options
 Thanks(2) Thanks(2)
 Quote Quote  Reply Reply
 Posted: May 05 2014 at 10:01pm Posted: May 05 2014 at 10:01pm |
|
Please call in and listen, if you can! These are the heavy-hitters in my field.
CDC Update for Clinicians on Middle East Respiratory Syndrome Coronavirus (MERS-CoV) Date: Tuesday, May 6, 2014 Tomorrow Time: 2:00 - 3:00 pm (Eastern Time) Audio Only: There are no presentation slides and registration is not required.
Passcode: 6525394 Overview: Middle East Respiratory Syndrome Coronavirus (MERS-CoV) is a virus that has caused severe respiratory illness and death in the Middle East. Epidemiologic investigations have demonstrated that this virus spreads from person to person during close contact, such as within families and healthcare facilities. The first case of imported MERS-CoV was reported last week in the state of Indiana. Clinicians have a critical role in recognizing and managing suspected cases of MERS-CoV. During this COCA Call, CDC subject matter experts will discuss the epidemiology, clinical signs, and infection control recommendations for MERS-CoV. Presenter(s): Susan Gerber, MD Medical Epidemiologist Division of Viral Diseases National Center for Immunization and Respiratory Diseases ─ CDC Marty Cetron, MD Director Division of Global Migration and Quarantine National Center for Emerging and Zoonotic Diseases ─ CDC David Kuhar, MD Medical Officer Division of Healthcare Quality Promotion National Center for Emerging and Zoonotic Diseases ─ CDC For additional information and to access call recordings (audio and transcript), which will be available a few days after the live call, please visit the call webpage athttp://emergency.cdc.gov/coca/calls/2014/callinfo_050614.asp If you have questions or trouble accessing this COCA Call, please e-mail coca@cdc.gov. |
|
|
CRS, DrPH
|
|
 |
|
Post Reply 
|
|
|
Tweet
|
| Forum Jump | Forum Permissions  You cannot post new topics in this forum You cannot reply to topics in this forum You cannot delete your posts in this forum You cannot edit your posts in this forum You cannot create polls in this forum You can vote in polls in this forum |